When data save lives
Using data that come from various and sometimes heterogeneous origins and sources represents a very promising area of medical research.
Using data that come from various and sometimes heterogeneous origins, sources (and formats, and which are generally not in a coherent, combined form) represents a very promising area of medical research. When these data are restructured and cross-referenced, mutual enrichment takes place and they become a real asset when seeking to make therapeutic progress.
When studying COVID-19, for example, researchers used databases consisting of reimbursement requests made to insurance companies and demographic and lifestyle-related data produced by credit institutions and governments. These data, alongside those produced by laboratories, have been and are still being used to support studies of how COVID-19 affects specific groups of people and to predict hospitalization rates.
However, when we talk about the widespread use of cross-referenced, restructured and aggregated data, we immediately run into the question of confidentiality. Data do not consist of abstract figures but are intimately linked to the experiences of patients and citizens. The use of personal data must be clearly circumscribed; but if the rules are too strict, this will prevent effective use of the data; for exemple, if rules prevent singularization, correlation and inference.
Singularization means the ability to identify, within a group, the person to which the data refer. Correlation means the ability to connect data from various sources to a single person. And inference means the ability to deduce something about a person simply because he or she is part of a group. Even if the person in question cannot be named, the data set cannot be regarded as anonymous if any of these three elements is possible.
Maintaining medical secrecy and confidentiality
In addition, pharmaceutical and IT companies are working on solutions that allow people to take part in studies remotely or from home. As a result, new issues are raised around obtaining patient identification and consent, as well as maintaining medical secrecy and confidentiality. Remote services must take place with the same level of confidentiality as if they were happening face-to-face behind closed doors in the doctor’s office or clinic. Complete segregation of the data, involving both physical and logical separation, is probably part of the solution.
When carrying out clinical trials, major pharmaceutical companies send personal data around the world, for example, in order to submit data to regulators and to comply with legislation. After marketing authorization has been obtained, data from several countries must be assessed for pharmacovigilance purposes. As a result, legal ways of transferring data, for example from the European Union to the United States, are needed.
Informed patient consent
When patients take part in a clinical trial, they go through several stages, starting with the informed consent process. Thirty-five percent of potential patients refuse to take part in a clinical trial because they say that they cannot understand the information provided to them. Patients using paper-based consent systems show a lower rate of understanding than those using electronic consent systems, which allow information to be provided via various modes of communication.
With eConsent – the electronic, remote consent solution developed by MEDIDATA – patients spend more time finding out about the clinical trial and gain a better understanding of the aims, advantages and risks of a study and of their own rights and responsibilities. This means that eConsent improves both patient education and patient commitment, and also leads to greater compliance and retention rates during the study.
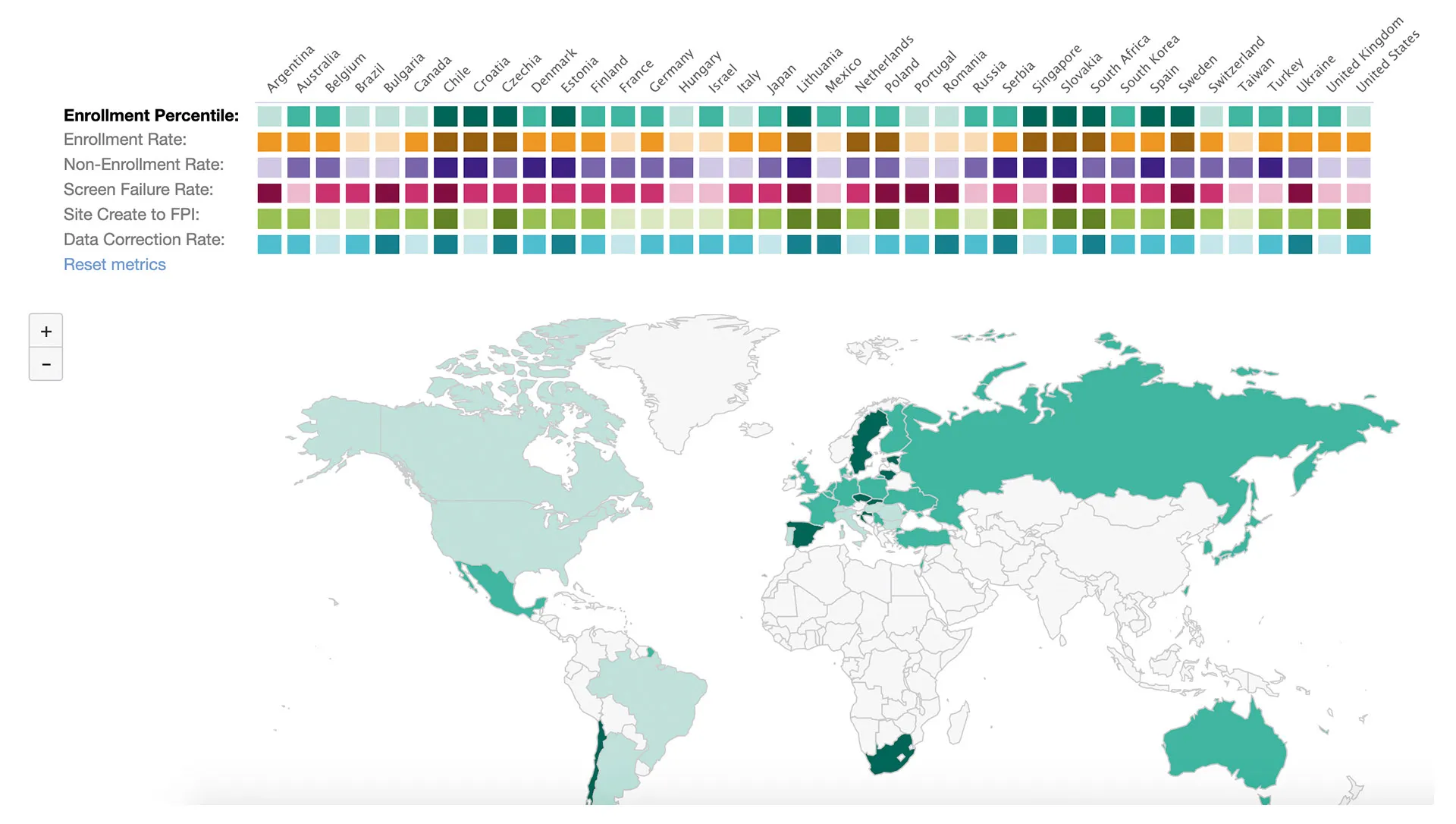
Processing and using data
MEDIDATA subsidiary Acorn AI uses unparalleled clinical data, advanced analytics and deep human expertise developed over 20 years to propel life sciences companies growth by accelerating insights and speed to market. In particular, the Intelligent Trial solution provides cross-industry, real time operational clinical trial data, enabling customers to gain a competitive edge as they execute clinical trials with increased agility.
Synthetic Control Arm®, MEDIDATA’s external control arm solution, uses historical, cross-industry patient-level clinical trial data to replace or supplement control arms, especially in diseases lacking clinical equipoise. Thus, Synthetic Control Arm can speed clinical development in situations in which traditional randomized controlled trials are not feasible, or impose undue patient burden.
After acquisition and processing, the use of synthetic control arm also requires special expertise in the data. MEDIDATA Detect is a centralized statistical analysis tool whose algorithms help researchers assess clinical data by focusing on their quality and patient safety. In particular, the solution allows data to be standardized, aggregated and collated from different, complex user experiences and from disparate and heterogeneous sources.
MEDIDATA has simplified these advanced analyses by adopting a platform approach, with data being transferred automatically to the cloud, without it being necessary to extract or upload data.
The European Data Protection Board sets out the legal bases on which we can rely for the data processing.